Autism Spectrum Disorder: “Children of the Rain”
For the average person, when the term “autism spectrum disorder” (ASD) is mentioned, the image of the main character from the film “Rain Man” will most likely come to mind, and that’s about it. In the post-Soviet space, the topic of ASD is not covered sufficiently, and diagnostics in most cases are far from perfect [1]. Every year in the world, the number of children with autism spectrum disorders is increasing.
Doctors talk about different reasons: improved diagnostic systems, suspicion of the influence of early vaccination, harmful effects of the notorious GMOs, and even the older age of future fathers. So what is ASD and what have scientists already managed to learn about the causes of its development?
What is ASD (autism spectrum disorders)?
Autism spectrum disorder (ASD) is a nervous system disorder characterized by deficits in social interactions and communication with the presence of stereotypies (repetitive actions) [2], and according to United States data for 2014, it is diagnosed in one out of 59 children [3].
ASD is diagnosed in all racial, ethnic, and socioeconomic groups, occurring five times more often in boys than in girls [4].
At present, the causes of the disease are not known, but it is assumed that it arises as a result of complex interactions between genetic, epigenetic, and environmental factors [5], [6] (Fig. 1).
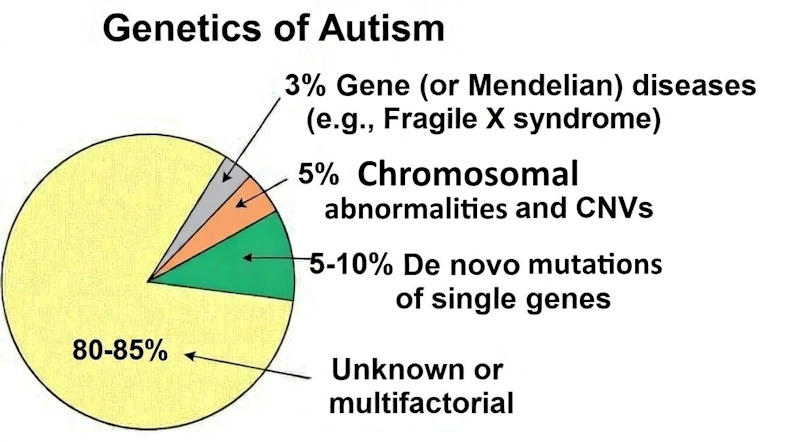
Figure 1. Genetics of Autism diagram. Image: re-cognition.center
Until May 2013, the official diagnoses of the autism spectrum in the American “Diagnostic and Statistical Manual of Mental Disorders” (DSM) included:
- autistic disorder;
- pervasive developmental disorder not otherwise specified (PDD-NOS);
- childhood disintegrative disorder;
- Rett syndrome;
- Asperger’s syndrome.
Today, in the latest, fifth edition of the DSM, there exists only one diagnosis – “autism spectrum disorder” with three degrees of severity, but many therapists, clinicians, parents, and organizations continue to use such terms as PDD-NOS and Asperger’s syndrome [2].
Symptoms
Autism spectrum disorder is often characterized by problems in the social, communicative, and intellectual abilities of patients. Depending on age and intellect, children with autism show varying degrees of communication deficit. These deficits manifest in speech delays, monotonous speech, echolalia (uncontrolled automatic repetition of words heard in someone else’s speech), and also vary from poor understanding to complete absence of oral speech.
Nonverbal communication is also impaired and may include difficulties in establishing eye contact, difficulties in understanding facial expressions and gestures.
Another important feature of people with ASD is a deficit in social-emotional reciprocity (Fig. 2) [7].
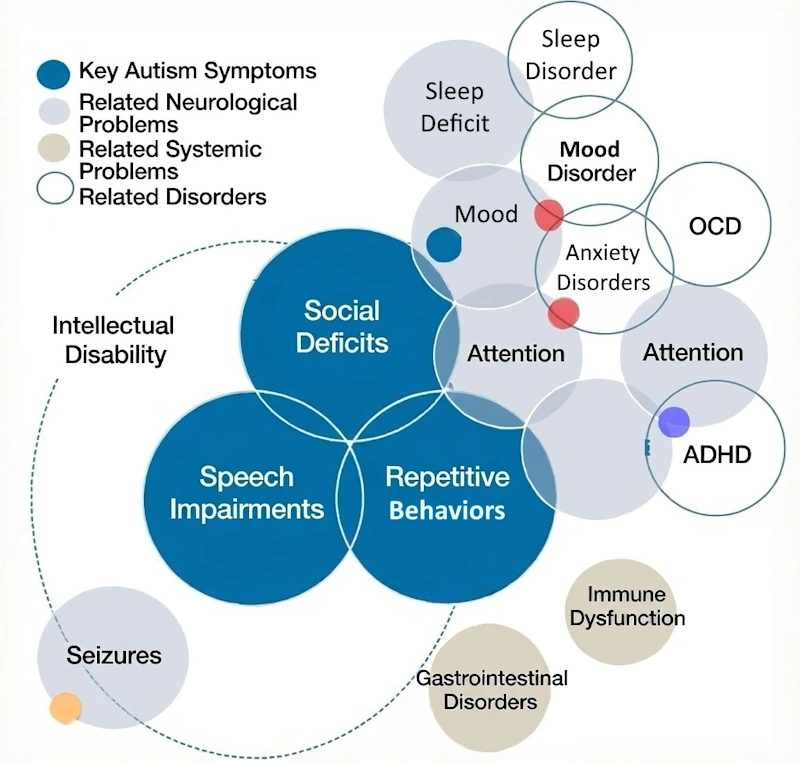
Figure 2. Symptoms of Autism Spectrum Disorders. Image: re-cognition.center
In simpler terms, children with autism spectrum disorder are not interested in communicating with people, understand them poorly, like to adhere to various rituals, are prone to repetitive body movements, may have language problems and delays in intellectual development.
Various symptoms lead to significant deterioration in many areas of adaptive functioning. At the same time, children with ASD often have many strengths:
- perseverance,
- attention to detail,
- good visual and mechanical memory,
- inclination toward monotonous work, which can be useful in some professions.
History of the condition
The term “autism” has been used for more than 100 years (since 1908). It was first voiced by Eugen Bleuler, a Swiss psychiatrist, and was used to describe patients with schizophrenia who were particularly self-absorbed. The term autism, which Bleuler used, comes from the Greek word autós, which means “self.” It was intended to describe the “isolated self” that he saw in people with schizophrenia [8].
In fact, these diagnoses are different, since a child with autism does not have hallucinations, delusions, they do not use speech to convey their irrational thoughts, because they often do not use speech at all.
Moreover, children with ASD have stable symptoms throughout their lives, while the diagnosis of “schizophrenia” usually implies periods of remission.
In 1943, a doctor named Leo Kanner conducted observations of groups of children who were previously considered mentally retarded. He noted that the children had difficulties in social interaction, anxiety when deviating from their usual way of life, echolalia, limited repertoire of spontaneous activity, but at the same time good intellectual potential, decent memory, hypersensitivity to sensory influences.
Kanner is credited with introducing the term “early infantile autism” (EIA) to describe the set of symptoms in the children he studied [8].
German scientist Hans Asperger in 1944 described a “milder” form of autism, which until today was known as Asperger’s syndrome. He described cases with boys who were very intelligent but had problems with social interactions. He noted difficulties with eye contact in children, stereotyped words and movements, as well as resistance to changes, but at the same time they had no deficiencies in speech and language education.
Unlike Kanner, Asperger also noted coordination problems in these children, but at the same time more abilities for abstract thinking.
Unfortunately, Asperger’s research was discovered only three decades later, when people began to question the diagnostic criteria used at that time. Only in the 1980s was Asperger’s work translated into English, published, and became known [8], [9].
In 1967, psychiatrist Bruno Bettelheim wrote that autism has no organic basis but is the result of upbringing by mothers who consciously or unconsciously did not want their children, which in turn led to restraint in relationships with them.
He claimed that the main cause of the disease was negative parental attitude toward infants at critical early stages of their psychological development [10].
Bernard Rimland, a psychologist and father of a child with autism, disagreed with Bettelheim. He could not accept the thought that the cause of his son’s autism was either his parenting mistakes or those of his wife.
In 1964, Bernard Rimland published the work “Infantile Autism: The Syndrome and Its Implications for a Neural Theory of Behavior,” which indicated the direction for further research at that time [8].
Autism became better known in the 1970s, but at that time many parents still confused autism with mental retardation and psychosis. Scientists began to bring clarity to the etiology of the disease: a 1977 study on twins showed that autism is largely determined by genetics and biological differences in brain development [10].

Scientists who studied autism. Image: re-cognition.center
In 1980, the diagnosis “infantile autism” was first included in the “Diagnostic and Statistical Manual of Mental Disorders” (DSM); the disease was also officially separated from childhood schizophrenia. In 1987, the DSM replaced “infantile autism” with the broader definition “autistic disorder” and included it in the revised third edition.
At the same time, psychologist and Doctor of Philosophy Ivar Lovaas published the first study showing how intensive behavioral therapy can help children with autism, which gave parents new hope (Fig. 3) [8], [9].
In 1994, Asperger’s syndrome was added to the DSM, expanding the diagnoses of the autism spectrum, thus including more “mild” cases [10].
In 1998, a study was published about the measles, mumps, and rubella (MMR) vaccine causing autism. The results of this study were refuted, but it attracted enough attention to cause confusion to this day (Fig. 4) [9]. Today there is no scientific data confirming a link between vaccination and ASD [11]. Sadly, quite recently, in August 2018, a report came out saying that more than 50% of people in some European countries still believe that vaccines cause autism [12].
Finally, in 2013, DSM-5 combined all subcategories of the condition into one diagnosis “autism spectrum disorder,” and Asperger’s syndrome is no longer considered a separate condition [8–10].
Causes of ASD
The precise underlying cause of autism spectrum disorder (ASD) remains unidentified. It can arise as a result of genetic predisposition, environmental or unknown factors, that is, ASD is not etiologically homogeneous. There are probably many subtypes of ASD, each of which has a different origin.
Genetics
It is assumed that the development of ASD is largely associated with the influence of genetic factors. In support of genetics as a cause, we can add the results of studies showing that ASD is more common in boys than in girls, which is most likely caused by genetic differences associated with the Y chromosome [14]. Studies of twins with ASD also speak in favor of the theory, which determined concordance rates (concordance is the presence of a certain trait in both twins) for monozygotic (60–90%) and dizygotic (0–10%) twins [15].
High concordance in pairs of monozygotic twins and significantly lower concordance in pairs of dizygotic twins indicate a significant role of genetic factors. A 2011 study found that nearly one in five infants who had an older biological sibling diagnosed with ASD were also diagnosed with the condition, and the likelihood increased further when multiple older siblings were affected [16].
Researchers have calculated that there are 65 genes that are considered strongly associated with autism, and 200 genes that are more weakly associated with this diagnosis [17]. Genome-wide association studies (GWAS) confirm the contribution of common allelic variance to ASD, including single nucleotide polymorphisms (SNP) and copy number variations (CNV) [18].
When examining the parents of patients, a large contribution of de novo CNV to ASD was discovered [19] (de novo mutations, or variations, are mutations that were not present in any family members and appeared for the first time in the patient).
According to research published in 2014, around 30% of individuals with the disorder show genetic changes linked to de novo mutations and variations in copy number (CNVs) [20].
Analysis of data from 1,000 families in 2011 linked two chromosomal regions, 7q11.23 and 16p11.2, with autism [21], but in 2015 Sanders and his colleagues, studying 10,220 people from 2,591 families, showed [17] that CNVs in four more regions are equally likely to be real candidates for variations associated with autism.
In September 2018, an article came out reporting that Japanese people with autism and schizophrenia have overlapping CNVs [22].
Recent studies of ASD cohorts report relatively high rates of de novo mutations in non-coding regions of the genome, as well as small exome mutations, that is, coding regions of the genome, which include both known and previously undetected candidate genes associated with ASD (Fig. 5) [23], [24].
Neurobiological factors
Genetic abnormalities can lead to abnormal brain development mechanisms, which in turn leads to its structural and functional, as well as cognitive and neurobiological disorders. Neurobiological differences associated with ASD diagnosis include structural and functional pathologies of the brain, including:
- enlarged gray matter in the frontal and temporal lobes [25];
- reduced white matter compared to gray matter in adolescence [26];
- anatomical and functional differences in the cerebellum and limbic system [26].
Researchers in 2018 discovered that boys with ASD have a smaller fractal dimension (a measure of structural complexity of an object) in the right part of the cerebellum than healthy children [27].
Some studies focus on the hypothesis that disrupted interactions between brain areas are the main cause of ASD development [28], while other researchers study molecular causes, such as impairments in the functioning of certain types of neurons (for example, mirror neurons) or disruptions in neurotransmission (signal transmission between neurons) [29].
Other causes
More and more researchers are writing about environmental causes that may contribute to autism. Studies have identified a number of potentially dangerous substances that may be associated with children autism development:
- lead,
- polychlorinated biphenyls (PCBs),
- insecticides,
- automobile exhaust,
- hydrocarbons,
- flame retardants [25]
However, for none of these substances has a trigger effect on the occurrence of ASD been proven.
There is also growing interest in the role of the immune system in the etiology of the disease. A report from June 2018 revealed that food allergies were present in 11.25% of children diagnosed with ASD, a rate markedly higher than the 4.25% observed among children without the condition, which can be added to the growing body of evidence pointing to immunological dysfunction as a possible risk factor for ASD [30].
Recent studies have also linked deficiencies in the diet of pregnant mothers and the presence of elevated levels of pesticides in the blood with the presence of ASD diagnosis in their children [31–33].
Diagnosis
A child with developmental delays should be examined by a doctor with the aim of finding the cause of the developmental delay. If the child exhibits any symptoms of autism spectrum disorder, they will most likely be referred to specialists for consultation, for example, to a child psychiatrist, child psychologist, pediatric neurologist.
For proper diagnosis, one must consider the complete patient history, physical examination, neurological examination, and direct assessment of the child’s social, language, and cognitive development. Sufficient time must be provided for standardized parent interviews regarding current problems and behavior history, as well as structured observation of social and communicative behavior, play.
According to a new 2018 study, a new blood test can detect about 17% of children with ASD. Scientists identified a group of blood metabolites that could help detect some children with autism spectrum disorder. As part of the “Children’s Autism Metabolome Project” (CAMP), the largest ASD metabolomics study, these results are a key step toward developing a biomarker test for ASD [34].
In August 2018, researchers reported differences in gene expression of bacteria in the oral area that could distinguish children with ASD from their healthy peers. The study suggests that gut microbiome disruptions previously identified in children with ASD may extend to the mouth and throat [35].
Scientists at the University of Missouri School of Medicine and the M.U. Thompson Center for Autism and Neurodevelopmental Disorders in June 2018 identified a link between neurotransmitter imbalance and the characteristics of connections between brain regions that play a role in social communication and language. The study described two tests that could lead to more accurate treatment [36].
Treatment
Treatment used in the 60s and 70s consisted of taking LSD, applying electric current, and rigid control of the patient’s behavior, which often included pain and punishment. Only in the 80s and 90s did doctors begin to implement more modern methods of treating children with autism, such as behavioral therapy with an emphasis on positive reinforcement and training under constant supervision [9].
Today, treatment can include both psychotherapy and medication. Many people with autism have additional symptoms such as sleep disturbances, seizures, and gastrointestinal problems.
Treatment of these symptoms can improve patients’ attention, learning, and related behavior. Some medications used for other conditions help with certain symptoms: antipsychotics (risperidone and aripiprazole), antidepressants, stimulants, anticonvulsants [37].
Currently, risperidone and aripiprazole are the only drugs approved by the FDA (Food and Drug Administration, USA) for symptoms associated with autism spectrum disorders, considering the irritability often observed with this diagnosis. Children and adolescents with autism spectrum disorder appear to be more susceptible to side effects when using medications, so the use of small doses is recommended [38].
Among non-medication treatments, applied behavior analysis, cognitive-behavioral therapy, social skills training, sensory integration therapy, occupational therapy, and speech therapy are currently used [35].
Children with autism spectrum disorders can have strengths too. Their unique perspectives on the world give other people the opportunity to see the world from a different side, children with ASD can grow into talented and successful people who will make remarkable discoveries to improve our world. New research in the field of diagnosis and treatment of “children of the rain” gives these unusual children hope for more successful social adaptation and even recovery.
Literature
- “If the number of people with ASD is unknown — it is too easy to ignore autism”. (2017). “Exit”;
- American Psychiatric Association Diagnostic and Statistical Manual of Mental Disorders — American Psychiatric Association, 2013;
- Jon Baio, Lisa Wiggins, Deborah L. Christensen, Matthew J Maenner, Julie Daniels, et. al.. (2018). Prevalence of Autism Spectrum Disorder Among Children Aged 8 Years — Autism and Developmental Disabilities Monitoring Network, 11 Sites, United States, 2014. MMWR Surveill. Summ.. 67, 1-23;
- Baio J. (2012). Prevalence of autism spectrum disorders — Autism and developmental disabilities monitoring network, 14 Sites, United States, 2008. MMWR. 61, 1–19;
- Hristo Y. Ivanov, Vili K. Stoyanova, Nikolay T. Popov, Tihomir I. Vachev. (2015). Autism Spectrum Disorder – A Complex Genetic Disorder. Folia Medica. 57, 19-28;
- Simashkova N.V. and Makushkin E.V. (2015). Autism spectrum disorders: diagnosis, treatment, observation. Russian Society of Psychiatrists;
- Lisa Campisi, Nazish Imran, Ahsan Nazeer, Norbert Skokauskas, Muhammad Waqar Azeem. (2018). Autism spectrum disorder. British Medical Bulletin. 127, 91-100;
- Mandal A. (2018). Autism history. News-Medical.Net;
- Ames C. (2018). What is the history of autism spectrum disorder? Harkla;
- The history of autism. (2014). Parents;
- The world before and after the invention of vaccines;
- Duffy B. (2018). Autism and vaccines: more than half of people in Britain, France, Italy still think there may be a link. The Conversation;
- Olson S. (2014). History of autism and vaccines: how one man unraveled the world’s faith In vaccinations. Medical Daily;
- Suniti Chakrabarti, Eric Fombonne. (2005). Pervasive Developmental Disorders in Preschool Children: Confirmation of High Prevalence. AJP. 162, 1133-1141;
- A. Bailey, A. Le Couteur, I. Gottesman, P. Bolton, E. Simonoff, et. al.. (1995). Autism as a strongly genetic disorder: evidence from a British twin study. Psychol. Med.. 25, 63;
- S. Ozonoff, G. S. Young, A. Carter, D. Messinger, N. Yirmiya, et. al.. (2011). Recurrence Risk for Autism Spectrum Disorders: A Baby Siblings Research Consortium Study. PEDIATRICS;
- Stephan J. Sanders, Xin He, A. Jeremy Willsey, A. Gulhan Ercan-Sencicek, Kaitlin E. Samocha, et. al.. (2015). Insights into Autism Spectrum Disorder Genomic Architecture and Biology from 71 Risk Loci. Neuron. 87, 1215-1233;
- Lauren A. Weiss, Dan E. Arking, Mark J. Daly, Aravinda Chakravarti, Dan E. Arking, et. al.. (2009). A genome-wide linkage and association scan reveals novel loci for autism. Nature. 461, 802-808;
- Anne B Arnett, Sandy Trinh, Raphael A Bernier. (2019). The state of research on the genetics of autism spectrum disorder: methodological, clinical and conceptual progress. Current Opinion in Psychology. 27, 1-5;
- Ivan Iossifov, Brian J. O’Roak, Stephan J. Sanders, Michael Ronemus, Niklas Krumm, et. al.. (2014). The contribution of de novo coding mutations to autism spectrum disorder. Nature. 515, 216-221;
- Dan Levy, Michael Ronemus, Boris Yamrom, Yoon-ha Lee, Anthony Leotta, et. al.. (2011). Rare De Novo and Transmitted Copy-Number Variation in Autistic Spectrum Disorders. Neuron. 70, 886-897;
- Itaru Kushima, Branko Aleksic, Masahiro Nakatochi, Teppei Shimamura, Takashi Okada, et. al.. (2018). Comparative Analyses of Copy-Number Variation in Autism Spectrum Disorder and Schizophrenia Reveal Etiological Overlap and Biological Insights. Cell Reports. 24, 2838-2856;
- Tychele N. Turner, Fereydoun Hormozdiari, Michael H. Duyzend, Sarah A. McClymont, Paul W. Hook, et. al.. (2016). Genome Sequencing of Autism-Affected Families Reveals Disruption of Putative Noncoding Regulatory DNA. The American Journal of Human Genetics. 98, 58-74;
- Ryan K C Yuen, Daniele Merico, Matt Bookman, Jennifer L Howe, Bhooma Thiruvahindrapuram, et. al.. (2017). Whole genome sequencing resource identifies 18 new candidate genes for autism spectrum disorder. Nat Neurosci. 20, 602-611;
- Autism. American Speech-Language-Hearing Association;
- Fred R. Volkmar, Catherine Lord, Anthony Bailey, Robert T. Schultz, Ami Klin. (2004). Autism and pervasive developmental disorders. J Child Psychol & Psychiat. 45, 135-170;
- Guihu Zhao, Kirwan Walsh, Jun Long, Weihua Gui, Kristina Denisova. (2018). Reduced structural complexity of the right cerebellar cortex in male children with autism spectrum disorder. PLoS ONE. 13, e0196964;
- Ruth A. Carper, Eric Courchesne. (2005). Localized enlargement of the frontal cortex in early autism. Biological Psychiatry. 57, 126-133;
- R. Bernier, G. Dawson, S. Webb, M. Murias. (2007). EEG mu rhythm and imitation impairments in individuals with autism spectrum disorder. Brain and Cognition. 64, 228-237;
- Guifeng Xu, Linda G. Snetselaar, Jin Jing, Buyun Liu, Lane Strathearn, Wei Bao. (2018). Association of Food Allergy and Other Allergic Conditions With Autism Spectrum Disorder in Children. JAMA Network Open. 1, e180279;
- Nathanael J Yates, Dijana Tesic, Kirk W Feindel, Jeremy T Smith, Michael W Clarke, et. al.. (2018). Vitamin D is crucial for maternal care and offspring social behaviour in rats. Journal of Endocrinology. 237, 73-85;
- Johnathan R. Nuttall. (2017). The plausibility of maternal toxicant exposure and nutritional status as contributing factors to the risk of autism spectrum disorders. Nutritional Neuroscience. 20, 209-218;
- Alan S. Brown, Keely Cheslack-Postava, Panu Rantakokko, Hannu Kiviranta, Susanna Hinkka-Yli-Salomäki, et. al.. (2018). Association of Maternal Insecticide Levels With Autism in Offspring From a National Birth Cohort. AJP. 175, 1094-1101;
- Alan M. Smith, Joseph J. King, Paul R. West, Michael A. Ludwig, Elizabeth L.R. Donley, et. al.. (2018). Amino Acid Dysregulation Metabotypes: Potential Biomarkers for Diagnosis and Individualized Treatment for Subtypes of Autism Spectrum Disorder. Biological Psychiatry;
- Steven D. Hicks, Richard Uhlig, Parisa Afshari, Jeremy Williams, Maria Chroneos, et. al.. (2018). Oral microbiome activity in children with autism spectrum disorder. Autism Research. 11, 1286-1295;
- John P. Hegarty, Dylan J. Weber, Carmen M. Cirstea, David Q. Beversdorf. (2018). Cerebro-Cerebellar Functional Connectivity is Associated with Cerebellar Excitation–Inhibition Balance in Autism Spectrum Disorder. J Autism Dev Disord. 48, 3460-3473;
- Legg T.J. (2018). Autism treatment guide. Healthline;
- DeFilippis M. and Wagner K.D. (2016). Treatment of autism spectrum disorder in children and adolescents. Psychopharmacology Bulletin. 46, 18–41;
- Martien J. Kas, Jeffrey C. Glennon, Jan Buitelaar, Elodie Ey, Barbara Biemans, et. al.. (2014). Assessing behavioural and cognitive domains of autism spectrum disorders in rodents: current status and future perspectives. Psychopharmacology. 231, 1125-1146.
